- Aeviva
- Posts
- Burnout Doesn't Always Look Like You Think
Burnout Doesn't Always Look Like You Think
It is not always exhaustion. Sometimes it looks like cynicism, chronic illness, apathy, or feeling completely fine until you suddenly are not.

Most people picture burnout as a person slumped at their desk, unable to move.
That is one version.
What is less talked about: the high-functioning person who still meets every deadline but finds everything meaningless. The person who is not tired but is inexplicably angry at everything. The person who keeps getting sick with no explanation. The person whose gut has been a disaster for months.
Burnout has been officially recognized by the World Health Organization since 2019. It is defined as a syndrome resulting from chronic workplace stress that has not been successfully managed.
What the definition does not capture is how many shapes it takes before it becomes obvious.
Today's Issue
Main Topic: The four mechanisms by which a nuclear weapon damages and kills the human body, what each one does at the biological level, how far each effect reaches, and the evidence-based actions that meaningfully improve survival chances for those outside the immediate kill zone
Subtitles:
The four waves: how a nuclear weapon actually kills
Zone by zone: what happens to your body at each distance
Radiation sickness: what ionizing radiation does inside your cells
Fallout: the slow killer most people do not understand
What actually protects you: the science of shelter, timing, and decisions
Abstract: A nuclear detonation releases energy through four primary mechanisms: the fireball and direct blast (approximately 50% of total energy), thermal radiation or heat flash (approximately 35% of energy), ionizing radiation (approximately 5% prompt, 10% rToday's Issue
Main Topic: What burnout actually is biologically, the unexpected and often missed ways it presents, how it differs from depression, and what the science says about recovering from it
Subtitles:
What burnout does to your body: the biology behind the crash
The three dimensions of burnout and why exhaustion is only one of them
The presentations nobody talks about: when burnout looks like something else
Burnout vs depression: a distinction that matters clinically
What the science says about recovery
Abstract: Burnout is a psychological syndrome arising from chronic, unmanaged interpersonal and occupational stress, characterized by three dimensions described by researcher Christina Maslach: exhaustion (physical and emotional depletion), cynicism or depersonalization (increasing detachment and negative attitudes toward work and others), and inefficacy (reduced sense of personal accomplishment). The WHO's ICD-11 classification (2019) formally recognized it as an occupational phenomenon. Biologically, chronic burnout involves dysregulation of the HPA axis (hypothalamic-pituitary-adrenal axis, the brain-body stress communication system that controls cortisol release). In early burnout, cortisol tends to be elevated; in established or advanced burnout, a counter-intuitive pattern often emerges: the cortisol rhythm flattens, with a blunted cortisol awakening response (the normal spike in cortisol within 30-45 minutes of waking that sets alertness and energy for the day), producing a state described as hypocortisolism or "adrenal resilience impairment." This is not adrenal gland failure. It is functional recalibration of a system under chronic demand. Autonomic nervous system function is also consistently affected, with reduced heart rate variability (HRV) and chronically elevated sympathetic activation. Immunologically, burnout is associated with elevated pro-inflammatory cytokines (TNF-alpha, IL-6, CRP) and weakened immune surveillance, explaining the pattern of frequent infections many burned-out individuals notice.
Tech moves fast, but you're still playing catch-up?
That's exactly why 200K+ engineers working at Google, Meta, and Apple read The Code twice a week.
Here's what you get:
Curated tech news that shapes your career - Filtered from thousands of sources so you know what's coming 6 months early.
Practical resources you can use immediately - Real tutorials and tools that solve actual engineering problems.
Research papers and insights decoded - We break down complex tech so you understand what matters.
All delivered twice a week in just 2 short emails.
1. What Burnout Does to Your Body: The Biology Behind the Crash 🧬⚡
Burnout is not just a feeling. It is a measurable biological state.
The stress response in your body is run by a system called the HPA axis, which stands for hypothalamic-pituitary-adrenal axis.
In plain language: a chain of command running from a region of your brain (the hypothalamus), through a gland at the base of your skull (the pituitary), down to the adrenal glands sitting on top of your kidneys.
This system controls the release of cortisol, your primary stress hormone.
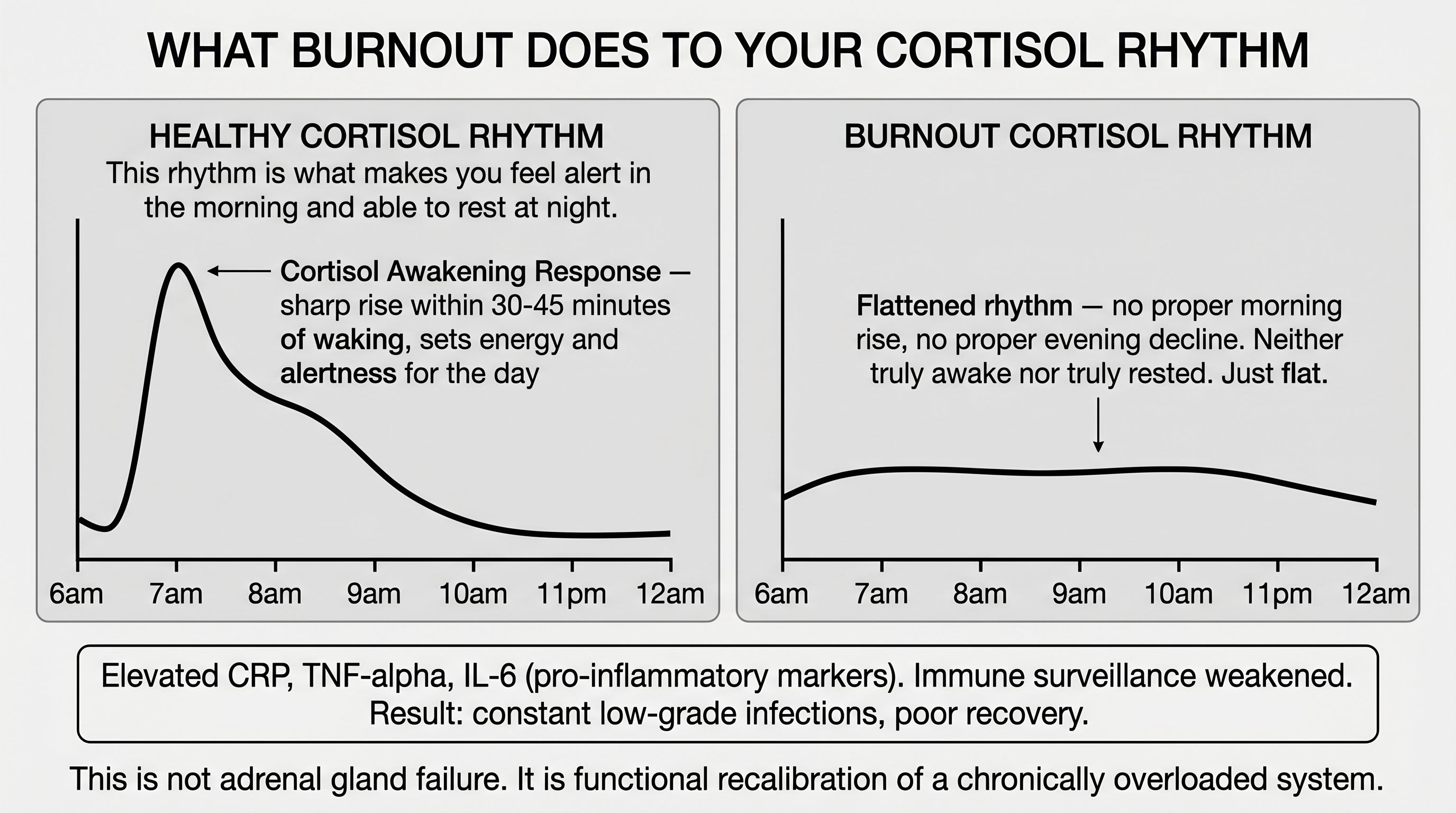
Under normal conditions, cortisol follows a daily rhythm. It spikes sharply within 30-45 minutes of waking (called the cortisol awakening response, which sets your alertness and energy for the day), then gradually falls through the afternoon and evening. This rhythm is what makes you feel alert in the morning and able to wind down at night.
In early burnout, cortisol levels tend to be elevated and erratic.
In established or advanced burnout, something counterintuitive happens: the rhythm flattens. The morning spike becomes blunted.
The system that was overactivated for so long begins to recalibrate downward. The result is a state where cortisol does not rise appropriately in the morning, does not fall appropriately at night, and does not respond properly to new stressors.
This is why burnout can make you feel neither truly awake nor truly rested. Neither on nor off. Just flat.
💡 Fun Fact: Burnout was first formally described as a clinical concept in 1974 by psychologist Herbert Freudenberger, who noticed a distinct pattern in himself and his colleagues at a free clinic in New York where they worked exhausting volunteer hours. He named it after the metaphor of a building burned out from the inside, structurally intact from the outside, hollow within.
2. The Three Dimensions of Burnout (and Why Exhaustion Is Only One of Them) 😮💨🧠

The WHO's definition of burnout names three dimensions. Most people only know one.
Exhaustion is the one everyone recognizes. Physical and emotional depletion. No energy. The tank is empty. This is what most people mean when they say they are burned out.
Cynicism (or depersonalization) is the second dimension, and it is far less discussed. This is a growing emotional distance from work, colleagues, or the people you are supposed to care about. It starts as detachment and progresses to contempt.
The nurse who starts to find patients annoying.
The teacher who stops caring whether students understand. The therapist who resents their clients.
Cynicism is the psyche's self-protective mechanism. When a person cannot leave a draining situation, they emotionally distance themselves from it.
The problem is that detachment spreads beyond work. Relationships outside work suffer. Interest in things that used to matter fades.
Inefficacy is the third dimension. A collapsing sense of competence.
The feeling that nothing you do makes a difference or is done well enough, even when objective performance may still be intact.
The reason this three-part framework matters: many people experiencing advanced burnout do not identify with "exhaustion" as their primary symptom. They are not tired. They are numb, cynical, and convinced they are failing. They may be working full hours and meeting deadlines. They may look completely fine from the outside.
3. The Presentations Nobody Talks About: When Burnout Looks Like Something Else 🎭⚠️

This is where burnout most commonly goes unrecognized.
Unexplained physical illness. Burnout suppresses the immune system while simultaneously elevating inflammation.
The practical result: constant low-grade infections, recurring headaches that do not respond to medication, persistent gut problems (IBS-like symptoms, nausea, appetite changes), heart palpitations with no cardiac cause, and dizziness. These are often investigated and treated as separate issues. They frequently are not.
Anger and irritability without fatigue. Burnout does not always produce tiredness. In high-performing individuals who continue to push through, the first prominent symptom is often a shortened fuse, disproportionate anger, and a plummeting tolerance for anything imperfect. This is often misread as a personality change, stress, or relationship problems.
Emotional numbness. Perhaps the least recognized presentation. A person who is not sad, not tired, not anxious, but who feels completely anesthetized. Nothing excites them. Nothing upsets them.
They go through the motions. This flat affect, an absence of emotional response to things that would normally produce one, is a hallmark of the depersonalization dimension of burnout, not a sign that everything is fine.
High-functioning burnout. Some people maintain output and performance well into advanced burnout, running on willpower, routine, and the identity investment of being "the one who handles everything." Their burnout is invisible until it is not, often manifesting suddenly as a physical collapse, illness, or a crisis that can no longer be managed. Performance as a signal of wellbeing is unreliable. Sometimes high performance is the last defense, not evidence of health.
4. Burnout vs Depression: A Distinction That Matters 🔍💊

These two conditions overlap substantially and can coexist. But they are clinically distinguishable in ways that affect treatment.
Context-specificity. Burnout is primarily tied to a specific context, usually work, caregiving, or another demanding role. A burned-out person may feel fine on holiday, energized by a weekend pursuing something they love, or normal in domains outside the one draining them.
Depression, in contrast, is pervasive. It follows you everywhere, affects every domain, and does not lift with context change alone.
Response to rest. Genuine rest and removal from the stressor can significantly reduce burnout symptoms.
True depression typically does not respond to rest in the same way. If two weeks of real vacation produces meaningful improvement, burnout is more likely the primary driver.
The cynicism signature. Depression rarely produces the specific pattern of contemptuous detachment toward others that cynicism in burnout does.
Depressed people often feel sad about people or disconnected from them. Burned-out people often feel contemptuous toward them.
The clinical concern: untreated burnout significantly increases the risk of developing clinical depression. The two conditions feed each other. And the longer burnout goes unaddressed, the harder the boundary between them becomes to find.
5. What the Science Says About Recovery 🔄🌱
The good news: the HPA axis recalibrates. The nervous system adapts. Burnout is not permanent.
The honest news: recovery is slower than most people expect, and returning to the same environment without structural change produces relapse.
What the evidence actually supports:
Real rest, not pseudo-rest. Scrolling your phone for three hours is not rest for a nervous system in chronic sympathetic overdrive. Recovery requires genuine downregulation: sleep, low-stakes physical activity (walking, swimming, yoga), nature exposure, and time genuinely free from performance demands. This is physiologically, not just psychologically, necessary.
Addressing the source, not just the symptoms. Recovery without changing the conditions that produced burnout is delay, not resolution. This means boundary-setting, workload adjustment, role change, or in some cases, leaving. No supplement or sleep routine compensates for a fundamentally unsustainable situation.
The cortisol rhythm rebuilds with consistent sleep schedules and morning light exposure. The cortisol awakening response, which flattens in burnout, is one of the most trainable aspects of HPA axis function.
Consistent wake times, morning sunlight within 30 minutes of waking, and reduced evening cortisol triggers (screens, high-stakes decisions, stimulants) have direct and measurable effects on cortisol rhythm restoration.
Seek a professional if you cannot distinguish burnout from depression. The distinction matters for treatment.
Depression requires intervention (therapy, medication, or both). Burnout may resolve with structural and lifestyle change. Trying to rest your way out of depression does not work. Trying to medicate your way out of pure burnout misses the source.

Takeaways
Burnout involves measurable biological changes: the HPA axis (the hypothalamus-pituitary-adrenal chain that controls cortisol) shifts from early overactivation to a flattened cortisol rhythm with a blunted morning awakening response, producing the characteristic flat, neither-on-nor-off feeling of advanced burnout, while simultaneously the immune system becomes pro-inflammatory and less effective at fighting infection, explaining the constant low-grade illness pattern most burned-out people notice but rarely connect to the burnout itself.
Burnout has three distinct dimensions: exhaustion (the one most people recognize), cynicism or depersonalization (emotional detachment and contempt, often the primary symptom in high-functioning individuals who maintain output), and inefficacy (collapsing sense of competence), and its most commonly missed presentations are physical symptoms (headaches, gut disruption, palpitations), disproportionate anger without fatigue, emotional numbness that looks like calm, and high-functioning performance that masks complete internal depletion until a sudden collapse.
Burnout is clinically distinguishable from depression by context-specificity (burnout is domain-linked, depression is pervasive) and response to rest (burnout improves with genuine removal from the stressor, depression does not), though untreated burnout significantly increases the risk of depression; recovery requires real downregulation of the nervous system, structural change to the conditions that caused it, and cortisol rhythm restoration through consistent sleep, morning light, and reduced evening stimulation.
Feedback & Sponsorship
What'd you think of this week's newsletter? Hit reply to let us know. Did we crush it? Blow your mind? We read every response.
Want your brand in front of hundreds of thousands of readers? Contact us for sponsorship opportunities [email protected]
Want more where that came from? Head to our website


Reply