- Aeviva
- Posts
- Next Time You're on Antibiotics, Don't Forget to Take Probiotics. Here's Why.
Next Time You're on Antibiotics, Don't Forget to Take Probiotics. Here's Why.
Antibiotics kill your gut bacteria indiscriminately. Probiotics during and after treatment can prevent diarrhea, yeast infections, and long-term microbiome damage
Estimated Read Time: 6 minutes
Antibiotics save lives by killing dangerous bacteria causing infections.
But they also kill the 100 trillion beneficial bacteria in your gut that digest food, produce vitamins, regulate immunity, and protect against disease.
Taking probiotics during and after antibiotics can prevent antibiotic-associated diarrhea (affects 30% of patients), restore gut health faster, and avoid long-term microbiome damage lasting months or years.
Today's Issue
Main Topic: Why antibiotics destroy your gut microbiome, how probiotics prevent side effects and speed recovery, and the exact protocol for taking them together
Subtitles:
How antibiotics damage your gut microbiome and why that matters
The benefits of taking probiotics with antibiotics (and the timing that matters)
Abstract: Antibiotics kill bacteria indiscriminately, eliminating not only pathogenic bacteria causing infections but also beneficial gut microbiota (100 trillion microorganisms performing essential functions including digestion, vitamin synthesis, immune regulation, pathogen resistance, and neurotransmitter production), with broad-spectrum antibiotics like amoxicillin, ciprofloxacin, and clindamycin reducing gut bacterial diversity by 25-50% within days and effects persisting 6-12+ months post-treatment if microbiome is not actively restored. Antibiotic-associated diarrhea (AAD) affects 5-35% of patients depending on antibiotic type, caused by disrupted gut flora allowing opportunistic pathogens (particularly Clostridioides difficile causing severe colitis) and reduced short-chain fatty acid production (beneficial bacteria ferment fiber producing butyrate, propionate, acetate that nourish colon cells and regulate inflammation). Probiotics taken concurrently with antibiotics reduce AAD risk by 50-60% (meta-analysis of 82 studies, 11,811 patients), prevent C. difficile infection, maintain beneficial species diversity, and accelerate microbiome recovery post-treatment. Optimal protocol involves taking probiotics containing Lactobacillus rhamnosus GG, Saccharomyces boulardii (yeast probiotic resistant to antibiotics), and Bifidobacterium species at doses 10-20 billion CFU, taken 2-3 hours AFTER antibiotic dose (timing prevents antibiotic from killing probiotic bacteria immediately), continuing throughout antibiotic course plus 2-4 weeks after completion to restore gut flora before stopping, combined with prebiotic fiber intake (15-25g daily from vegetables, fruits, whole grains feeding beneficial bacteria) supporting probiotic colonization and indigenous microbiome recovery.
The human gut microbiome (100 trillion bacteria, fungi, and other microorganisms in your gastrointestinal tract) performs critical functions: digesting fiber, synthesizing vitamins your body cannot produce, training your immune system (70% of immune cells reside in gut tissue), protecting against pathogens, and producing neurotransmitters affecting mood. When you take antibiotics (amoxicillin, azithromycin, ciprofloxacin, doxycycline), the drugs cannot distinguish between harmful bacteria causing infection and beneficial bacteria maintaining health, killing both indiscriminately. Broad-spectrum antibiotics reduce gut bacterial diversity by 25-50% within days, with changes persisting months or years if not actively restored. Consequences include diarrhea (5-35% of patients), C. difficile infection (life-threatening colitis when beneficial bacteria are eliminated), vaginal yeast infections (candida overgrowth), increased infection susceptibility, and potential metabolic changes. Probiotics taken concurrently prevent these complications through specific mechanisms and precise timing protocols that maximize benefits.

Gut Microbiome
Introducing the first AI-native CRM
Connect your email, and you’ll instantly get a CRM with enriched customer insights and a platform that grows with your business.
With AI at the core, Attio lets you:
Prospect and route leads with research agents
Get real-time insights during customer calls
Build powerful automations for your complex workflows
Join industry leaders like Granola, Taskrabbit, Flatfile and more.
1. What Antibiotics Do to Your Gut Bacteria Within Days 🦠💊
Antibiotics target bacterial functions like cell wall synthesis, protein production, or DNA replication.
Unfortunately, these mechanisms affect beneficial gut bacteria as effectively as pathogenic bacteria.
The destruction happens fast: Within 24-72 hours, gut populations decline dramatically. Ciprofloxacin reduces diversity by 30% in 3-4 days.
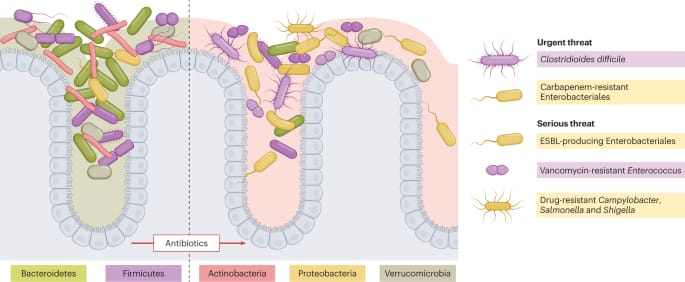
Antibiotic’s effect on Microbiome
Clindamycin cuts beneficial Bacteroides and Firmicutes by 50-90%, lasting 2+ years.
Amoxicillin-clavulanate eliminates protective Bifidobacterium and Lactobacillus while resistant pathogens proliferate.
Why it matters: Beneficial bacteria ferment fiber producing short-chain fatty acids (butyrate, propionate, acetate) that fuel colon cells, regulate inflammation, and maintain gut barrier.
They synthesize vitamins K, B12, folate, and biotin. They train 70-80% of your immune system.
They block pathogens through competitive exclusion and antimicrobial compounds. When antibiotics eliminate these species, you lose these protective functions.
2. The Most Common Side Effects: Diarrhea, C. Diff, and Yeast Infections 💩⚠️
Antibiotic-associated diarrhea (AAD): Affects 5-35% of patients. Highest risk: clindamycin (20-30%), amoxicillin-clavulanate (10-25%), cephalosporins (15-20%).
Caused by reduced SCFA production (colon cells starved), osmotic diarrhea (undigested carbs), and pathogen overgrowth.
C. difficile infection (CDI): Opportunistic bacterium causing severe colitis with profuse watery diarrhea, fever, abdominal pain, potentially fatal complications.
Occurs when antibiotics eliminate competitors allowing C. diff to proliferate and produce toxins.
Affects 5-10% hospitalized patients on antibiotics. Mortality 5-15% in severe cases.
Vaginal yeast infections: Antibiotics kill vaginal Lactobacillus (maintaining pH 3.8-4.5), allowing Candida overgrowth.
Affects 10-30% of women on antibiotics, especially broad-spectrum drugs.
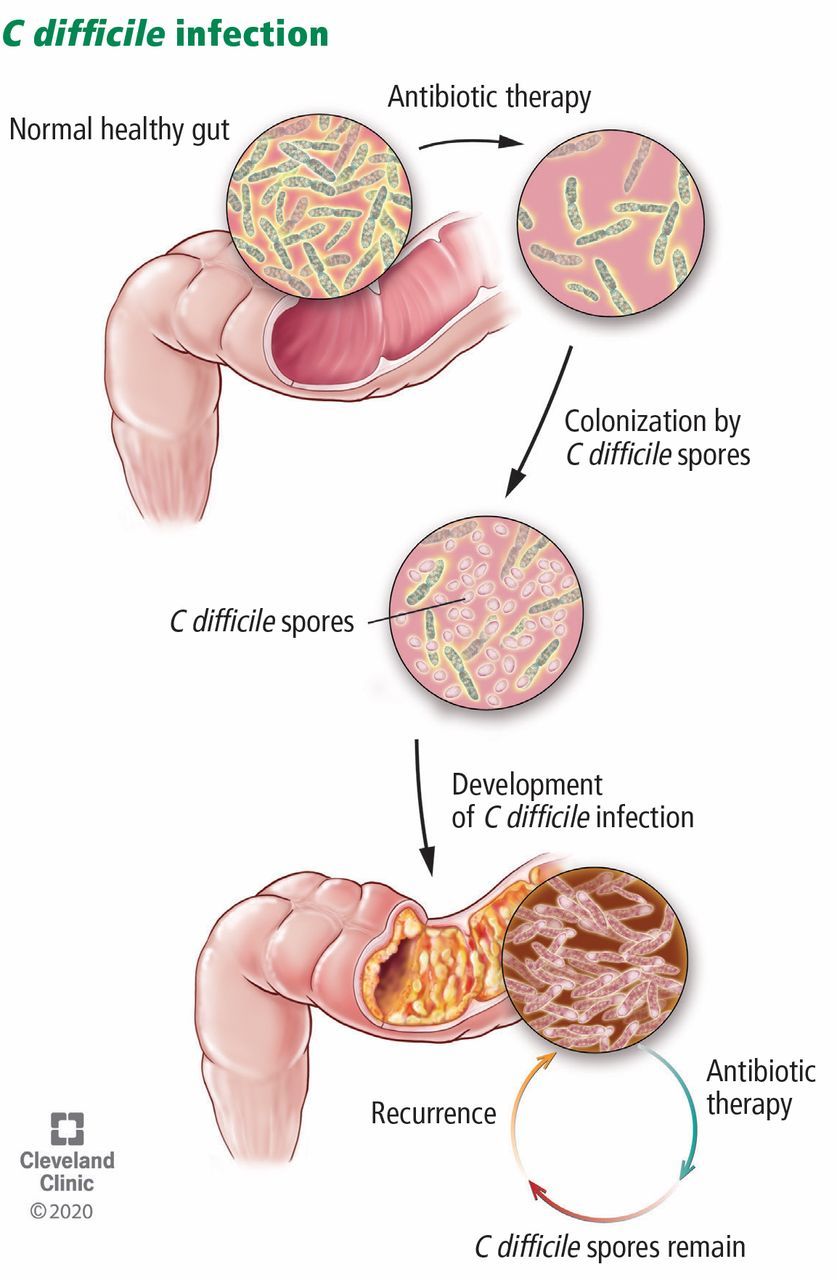
C. difficile infection
3. How Probiotics Prevent Antibiotic Damage (The Science) 🔬✅
Preventing diarrhea: 2012 Cochrane meta-analysis (82 trials, 11,811 patients) showed probiotics reduced AAD by 42%.
Diarrhea rates: 8% with probiotics vs 18% placebo. Number needed to treat: 10 patients need probiotics to prevent 1 case.
Most effective strains:
Lactobacillus rhamnosus GG: Reduces AAD by 50-64%. Survives stomach acid, produces antimicrobials.
Saccharomyces boulardii: Yeast probiotic (antibiotics do not kill it). Reduces AAD by 50-57%. Neutralizes C. diff toxins.
Bifidobacterium species: Reduce inflammation, produce SCFAs, support gut barrier.
Preventing C. diff: Probiotics reduce CDI risk by 60-70% in high-risk patients.
S. boulardii shows 50-84% reduction through competitive exclusion and toxin neutralization.
Maintaining diversity: DNA sequencing shows probiotics preserve beneficial species during antibiotic treatment, maintaining "seed populations" allowing faster recolonization (2-4 weeks vs 6-12+ months).
4. The Exact Timing Protocol: When and How to Take Probiotics With Antibiotics ⏰💊
The timing question: Will antibiotics kill probiotics? Partially yes, but timing solves this.
How it works: Antibiotics peak in gut 1-2 hours after dose, then decline over 6-12 hours. Taking probiotics SAME TIME kills most bacteria.
Solution: Take probiotics 2-3 hours AFTER antibiotic dose. Antibiotic concentration has declined enough for probiotics to colonize.
Example schedule:
8:00 AM: Antibiotic with breakfast
10:30 AM: Probiotic (2.5 hours later)
8:00 PM: Second antibiotic dose (if twice daily)
10:30 PM: Second probiotic dose

Why it works: Even if 50-70% die from residual antibiotic, surviving 30-50% produce metabolites, occupy niches preventing pathogens, stimulate immunity, and expand between doses.
S. boulardii advantage: Being yeast, antibiotics do not affect it. Can be taken anytime.
Complete protocol:
Strains: Multi-strain containing L. rhamnosus GG, S. boulardii, Bifidobacterium species
Dosage: 10-20 billion CFU per dose (20-50 billion for high-risk patients)
Duration: Throughout entire antibiotic course PLUS 2-4 weeks after finishing (critical for recovery)
Storage: Refrigerate most probiotics to maintain viability
5. Additional Strategies: Prebiotic Fiber, Fermented Foods, and Post-Antibiotic Recovery 🥗🦠
Prebiotic fiber (15-25g daily): Feeds beneficial bacteria and probiotics.
Sources: vegetables (onions, garlic, asparagus), fruits (bananas, apples), whole grains (oats), legumes. Supports surviving bacteria even during antibiotics.
Fermented foods: Yogurt (live cultures), kefir (30-50 strains), sauerkraut, kimchi, kombucha provide additional bacteria plus beneficial metabolites. Eat 1-2 servings daily.
Bone broth: Contains glutamine and glycine supporting gut lining integrity. 1-2 cups daily.
Avoid: Excessive sugar (feeds pathogens like candida, C. diff more than beneficial bacteria). Limit processed foods.
Hydration: 2-3 liters water daily, especially if experiencing diarrhea. Add electrolyte solutions if needed.
Post-antibiotic recovery: Continue probiotics 2-4 weeks after finishing antibiotics. Microbiome recovery continues for weeks. Extended supplementation accelerates restoration to baseline diversity.
When probiotics are MOST important: High-risk antibiotics (clindamycin, amoxicillin-clavulanate, fluoroquinolones), prolonged courses (10-14+ days), elderly patients (65+), recent antibiotic use within 3-6 months, history of AAD or C. diff.

💡 Pro Tip: Keep probiotics refrigerated and start them with your first antibiotic dose. Prevention beats treatment. Do not wait for diarrhea to develop.
Feel Better Today
If you feel stressed, anxious or depressed, you do not have to suffer alone. With BetterHelp, you can connect with a therapist who fits your needs and schedule. No commute, no waiting rooms - just real, meaningful help. Get started today - therapy has never been easier. Take 25% off your first month without HSA & FSA eligible service.
This email was delivered by a third-party, on behalf of BetterHelp. Copyright © 2025 BetterHelp. All Rights Reserved. 990 Villa St, Mountain View, California, United States.
Takeaways
Antibiotics kill gut bacteria indiscriminately, reducing diversity by 25-50% within days with effects lasting 6-12+ months if not restored, causing diarrhea (5-35% of patients), C. difficile infection, yeast infections, and weakened immunity from loss of 100 trillion beneficial microorganisms performing digestion, vitamin synthesis, and pathogen protection.
Probiotics during antibiotics reduce diarrhea by 42-60% and C. diff infection by 60-70% (82 studies, 11,811 patients), with most effective strains being Lactobacillus rhamnosus GG, Saccharomyces boulardii (yeast resistant to antibiotics), and Bifidobacterium species at 10-20 billion CFU doses.
Take probiotics 2-3 hours AFTER antibiotic doses (not simultaneously) throughout entire course plus 2-4 weeks after completion, combined with prebiotic fiber 15-25g daily, fermented foods, and hydration to restore gut flora in 2-4 weeks versus 6-12+ months without intervention.
Feedback & Sponsorship
What'd you think of this week's newsletter? Hit reply to let us know. Did we crush it? Blow your mind? We read every response.
Want your brand in front of hundreds of thousands of readers? Contact us for sponsorship opportunities [email protected]
Want more where that came from? Head to our website
Lose Up to 23% Body Weight
MedVi’s GLP-1 treatments are clinically proven to help patients lose up to 23% of their body weight. Get personalized medical support, proven medications, and a plan designed to deliver real, lasting results.
Read all warnings before using GLP-ls. Side-effects may include a risk of thyroid c-cell tumors. Do not use GLP-1s if you or your family have a history of thyroid cancer. In certain situations, where clinically appropriate, a provider may prescribe compounded medication, which is prepared by a state-licensed sterile compounding pharmacy partner. Although compounded drugs are permitted to be prescribed under federal law, they are not FDA-approved and do not undergo FDA review for safety, effectiveness, or manufacturing quality.




Reply